| CATEGORII DOCUMENTE |
| Bulgara | Ceha slovaca | Croata | Engleza | Estona | Finlandeza | Franceza |
| Germana | Italiana | Letona | Lituaniana | Maghiara | Olandeza | Poloneza |
| Sarba | Slovena | Spaniola | Suedeza | Turca | Ucraineana |
|
Functional Organization of the Human Body and Control of the 'Internal Environment' |
|
|
|
Human Physiology. In human physiology, we attempt to explain the specific characteristics and mechanisms of the human body that make it a living being. The very fact that we remain alive is almost beyond our control, for hunger makes us seek food and fear makes us seek refuge. Sensations of cold make us look for warmth. Other forces cause us to seek fellowship and to reproduce. Thus, the human being is actually an automaton, and the fact that we are sensing, feeling, and knowledgeable beings is part of this automatic sequence of life; these special attributes allow us to exist under widely varying conditions. |
|
|
|
|||||
|
Cells as the Living Units of the Body |
|||||||
|
The basic living unit of the body is the cell. Each organ is an aggregate of many different cells held together by intercellular supporting structures. |
|
Each type of cell is specially adapted to perform one or a few particular functions. For instance, the red blood cells, numbering 25 trillion in each human being, transport oxygen from the lungs to the tissues. Although the red cells are the most abundant of any single type of cell in the body, there are about 75 trillion additional cells of other types that perform functions different from those of the red cell. The entire body, then, contains about 100 trillion cells. |
|
Although the many cells of the body often differ markedly from one another, all of them have certain basic characteristics that are alike. For instance, in all cells, oxygen reacts with carbohydrate, fat, and protein to release the energy required for cell function. Further, the general chemical mechanisms for changing nutrients into energy are basically the same in all cells, and all cells deliver end products of their chemical reactions into the surrounding fluids. |
|
Almost all cells also have the ability to reproduce additional cells of their own kind. Fortunately, when cells of a particular type are destroyed from one cause or another, the remaining cells of this type usually generate new cells until the supply is replenished. |
|
Extracellular Fluid-The 'Internal Environment' |
|
page 3 |
|
|
|
page 4 |
|
About 60 per cent of the adult human body is fluid, mainly a water solution of ions and other substances. Although most of this fluid is inside the cells and is called intracellular fluid, about one third is in the spaces outside the cells and is called extracellular fluid. This extracellular fluid is in constant motion throughout the body. It is transported rapidly in the circulating blood and then mixed between the blood and the tissue fluids by diffusion through the capillary walls. |
|
In the extracellular fluid are the ions and nutrients needed by the cells to maintain cell life. Thus, all cells live in essentially the same environment-the extracellular fluid. For this reason, the extracellular fluid is also called the internal environment of the body, or the milieu intrieur, a term introduced more than 100 years ago by the great 19th-century French physiologist Claude Bernard. |
|
Cells are capable of living, growing, and
performing their special functions as long as the proper concentrations of
oxygen, glucose |
|
Differences Between Extracellular and
Intracellular Fluids. The extracellular fluid contains large amounts of sodium,
chloride, and bicarbonate ions plus nutrients for the cells, such
as oxygen, glucose |
|
The intracellular fluid differs significantly from the extracellular fluid; specifically, it contains large amounts of potassium, magnesium, and phosphate ions instead of the sodium and chloride ions found in the extracellular fluid. Special mechanisms for transporting ions through the cell membranes maintain the ion concentration differences between the extracellular and intracellular fluids. These transport processes are discussed in Chapter 4. |
|
'Homeostatic' Mechanisms of the Major Functional Systems |
|
Homeostasis |
|
The term homeostasis is used by physiologists to mean maintenance of nearly constant conditions in the internal environment. Essentially all organs and tissues of the body perform functions that help maintain these constant conditions. For instance, the lungs provide oxygen to the extracellular fluid to replenish the oxygen used by the cells, the kidneys maintain constant ion concentrations, and the gastrointestinal system provides nutrients. |
|
A large segment of this text is concerned with the manner in which each organ or tissue contributes to homeostasis. To begin this discussion, the different functional systems of the body and their contributions to homeostasis are outlined in this chapter; then we briefly outline the basic theory of the body's control systems that allow the functional systems to operate in support of one another. |
|
Extracellular Fluid Transport and Mixing System-The Blood Circulatory System |
|
Extracellular fluid is transported through all parts of the body in two stages. The first stage is movement of blood through the body in the blood vessels, and the second is movement of fluid between the blood capillaries and the intercellular spaces between the tissue cells. |
|
Figure 1-1 shows the overall circulation of blood. All the blood in the circulation traverses the entire circulatory circuit an average of once each minute when the body is at rest and as many as six times each minute when a person is extremely active. |
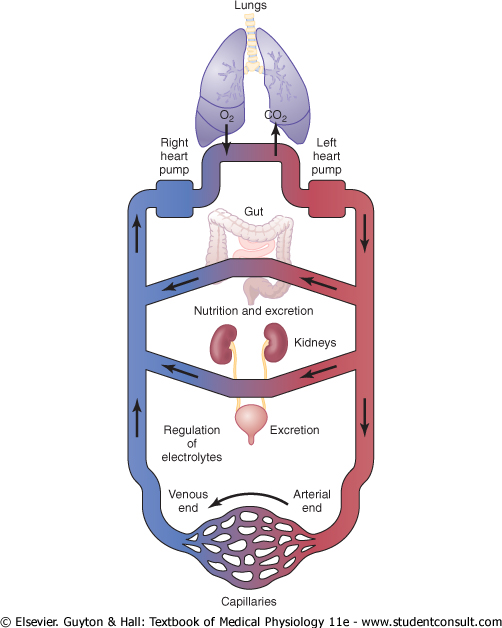
As blood passes through the blood capillaries, continual exchange of extracellular fluid also occurs between the plasma portion of the blood and the interstitial fluid that fills the intercellular spaces. This process is shown in Figure 1-2. The walls of the capillaries are permeable to most molecules in the plasma of the blood, with the exception of the large plasma protein molecules. Therefore, large amounts of fluid and its dissolved constituents diffuse back and forth between the blood and the tissue spaces, as shown by the arrows. This process of diffusion is caused by kinetic motion of the molecules in both the plasma and the interstitial fluid. That is, the fluid and dissolved molecules are continually moving and bouncing in all directions within the plasma and the fluid in the intercellular spaces, and also through the capillary pores. Few cells are located more than 50 micrometers from a capillary, which ensures diffusion of almost any substance from the capillary to the cell within a few seconds. Thus, the extracellular fluid everywhere in the body-both that of the plasma and that of the interstitial fluid-is continually being mixed, thereby maintaining almost complete homogeneity of the extracellular fluid throughout the body.
|
Origin of Nutrients in the Extracellular Fluid |
|
Respiratory System. Figure 1-1 shows that each time the blood passes through the body, it also flows through the lungs. The blood picks up oxygen in the alveoli, thus acquiring the oxygen needed by the cells. The membrane between the alveoli and the lumen of the pulmonary capillaries, the alveolar membrane, is only 0.4 to 2.0 micrometers thick, and oxygen diffuses by molecular motion through the pores of this membrane into the blood in the same manner that water and ions diffuse through walls of the tissue capillaries. |
|
Gastrointestinal Tract. A large portion of
the blood pumped by the heart also passes through the walls of the
gastrointestinal tract. Here different dissolved nutrients, including carbohydrates,
fatty acids, and amino acids |
|
Liver and Other Organs That Perform Primarily Metabolic Functions. Not all substances absorbed from the gastrointestinal tract can be used in their absorbed form by the cells. The liver changes the chemical compositions of many of these substances to more usable forms, and other tissues of the body-fat cells, gastrointestinal mucosa, kidneys, and endocrine glands-help modify the absorbed substances or store them until they are needed. |
|
Musculoskeletal System. Sometimes the question is asked, How does the musculoskeletal system fit into the homeostatic functions of the body? The answer is obvious and simple: Were it not for the muscles, the body could not move to the appropriate place at the appropriate time to obtain the foods required for nutrition. The musculoskeletal system also provides motility for protection against adverse surroundings, without which the entire body, along with its homeostatic mechanisms, could be destroyed instantaneously. |
|
Removal of Metabolic End Products |
|
Removal of Carbon Dioxide by the Lungs. At the same time that blood picks up oxygen in the lungs, carbon dioxide is released from the blood into the lung alveoli; the respiratory movement of air into and out of the lungs carries the carbon dioxide to the atmosphere. Carbon dioxide is the most abundant of all the end products of metabolism. |
|
Kidneys. Passage of the blood through the
kidneys removes from the plasma most of the other substances besides carbon
dioxide that are not needed by the cells. These substances include different
end products of cellular metabolism, such as urea |
|
The kidneys perform their function by first
filtering large quantities of plasma through the glomeruli into the tubules
and then reabsorbing into the blood those substances needed by the body, such
as glucose |
|
Regulation of Body Functions |
|
page 5 |
|
|
|
page 6 |
|
Nervous System. The nervous system is composed of three major parts: the sensory input portion, the central nervous system (or integrative portion), and the motor output portion. Sensory receptors detect the state of the body or the state of the surroundings. For instance, receptors in the skin apprise one whenever an object touches the skin at any point. The eyes are sensory organs that give one a visual image of the surrounding area. The ears also are sensory organs. The central nervous system is composed of the brain and spinal cord. The brain can store information, generate thoughts, create ambition, and determine reactions that the body performs in response to the sensations. Appropriate signals are then transmitted through the motor output portion of the nervous system to carry out one's desires. |
|
A large segment of the nervous system is called the autonomic system. It operates at a subconscious level and controls many functions of the internal organs, including the level of pumping activity by the heart, movements of the gastrointestinal tract, and secretion by many of the body's glands. |
|
Hormonal System of Regulation. Located in the body
are eight major endocrine glands that secrete chemical substances
called hormones. Hormones are transported in the extracellular fluid
to all parts of the body to help regulate cellular function. For instance,
thyroid hormone increases the rates of most chemical reactions in all cells,
thus helping to set the tempo of bodily activity. Insulin controls glucose |
|
Reproduction |
|
Sometimes reproduction is not considered a homeostatic function. It does, however, help maintain homeostasis by generating new beings to take the place of those that are dying. This may sound like a permissive usage of the term homeostasis, but it illustrates that, in the final analysis, essentially all body structures are organized such that they help maintain the automaticity and continuity of life. |
|
Control Systems of the Body |
|
The human body has thousands of control systems in it. The most intricate of these are the genetic control systems that operate in all cells to help control intracellular function as well as extracellular function. This subject is discussed in Chapter 3. |
|
Many other control systems operate within
the organs to control functions of the individual parts of the organs;
others operate throughout the entire body to control the interrelations
between the organs. For instance, the respiratory system, operating in
association with the nervous system, regulates the concentration of carbon
dioxide in the extracellular fluid. The liver and pancreas regulate the
concentration of glucose |
|
Examples of Control Mechanisms |
|
Regulation of Oxygen and Carbon Dioxide Concentrations in the Extracellular Fluid. Because oxygen is one of the major substances required for chemical reactions in the cells, it is fortunate that the body has a special control mechanism to maintain an almost exact and constant oxygen concentration in the extracellular fluid. This mechanism depends principally on the chemical characteristics of hemoglobin, which is present in all red blood cells. Hemoglobin combines with oxygen as the blood passes through the lungs. Then, as the blood passes through the tissue capillaries, hemoglobin, because of its own strong chemical affinity for oxygen, does not release oxygen into the tissue fluid if too much oxygen is already there. But if the oxygen concentration in the tissue fluid is too low, sufficient oxygen is released to re-establish an adequate concentration. Thus, regulation of oxygen concentration in the tissues is vested principally in the chemical characteristics of hemoglobin itself. This regulation is called the oxygen-buffering function of hemoglobin. |
|
Carbon dioxide concentration in the extracellular fluid is regulated in a much different way. Carbon dioxide is a major end product of the oxidative reactions in cells. If all the carbon dioxide formed in the cells continued to accumulate in the tissue fluids, the mass action of the carbon dioxide itself would soon halt all energy-giving reactions of the cells. Fortunately, a higher than normal carbon dioxide concentration in the blood excites the respiratory center, causing a person to breathe rapidly and deeply. This increases expiration of carbon dioxide and, therefore, removes excess carbon dioxide from the blood and tissue fluids. This process continues until the concentration returns to normal. |
|
page 6 |
|
|
|
page 7 |
|
Regulation of Arterial Blood Pressure. Several systems contribute to the regulation of arterial blood pressure. One of these, the baroreceptor system, is a simple and excellent example of a rapidly acting control mechanism. In the walls of the bifurcation region of the carotid arteries in the neck, and also in the arch of the aorta in the thorax, are many nerve receptors called baroreceptors, which are stimulated by stretch of the arterial wall. When the arterial pressure rises too high, the baroreceptors send barrages of nerve impulses to the medulla of the brain. Here these impulses inhibit the vasomotor center, which in turn decreases the number of impulses transmitted from the vasomotor center through the sympathetic nervous system to the heart and blood vessels. Lack of these impulses causes diminished pumping activity by the heart and also dilation of the peripheral blood vessels, allowing increased blood flow through the vessels. Both of these effects decrease the arterial pressure back toward normal. |
|
Conversely, a decrease in arterial pressure below normal relaxes the stretch receptors, allowing the vasomotor center to become more active than usual, thereby causing vasoconstriction and increased heart pumping, and raising arterial pressure back toward normal. |
|
|
|
Table 1-1 lists the more important constituents and physical characteristics of extracellular fluid, along with their normal values, normal ranges, and maximum limits without causing death. Note the narrowness of the normal range for each one. Values outside these ranges are usually caused by illness. |
|
Most important are the limits beyond which abnormalities can cause death. For example, an increase in the body temperature of only 11F (7C) above normal can lead to a vicious cycle of increasing cellular metabolism that destroys the cells. Note also the narrow range for acid-base balance in the body, with a normal pH value of 7.4 and lethal values only about 0.5 on either side of normal. Another important factor is the potassium ion concentration, because whenever it decreases to less than one third normal, a person is likely to be paralyzed as a result of the nerves' inability to carry signals. Alternatively, if the potassium ion concentration increases to two or more times normal, the heart muscle is likely to be severely depressed. Also, when the calcium ion concentration falls below about one half of normal, a person is likely to experience tetanic contraction of muscles throughout the body because of the spontaneous generation of excess nerve impulses in the peripheral nerves. When the glucose concentration falls below one half of normal, a person frequently develops extreme mental irritability and sometimes even convulsions. |
|
Table 1-1. Important Constituents and Physical Characteristics of Extracellular Fluid |
|
Normal Value |
|
Approximate Short-Term Nonlethal Limit |
Unit |
|
|
Oxygen |
mm Hg |
|||
|
Carbon dioxide |
mm Hg |
|||
|
Sodium ion |
|
mmol/L |
||
|
Potassium ion |
mmol/L |
|||
|
Calcium ion |
mmol/L |
|||
|
Chloride ion |
mmol/L |
|||
|
Bicarbonate ion |
mmol/L |
|||
|
Glucose |
mg/dl |
|||
|
Body temperature |
F (C) |
|||
|
Acid-base |
pH |
|
These examples should give one an appreciation for the extreme value and even the necessity of the vast numbers of control systems that keep the body operating in health; in the absence of any one of these controls, serious body malfunction or death can result. |
|
Characteristics of Control Systems |
|
The aforementioned examples of homeostatic control mechanisms are only a few of the many thousands in the body, all of which have certain characteristics in common. These characteristics are explained in this section. |
|
Negative Feedback Nature of Most Control Systems |
|
Most control systems of the body act by negative feedback, which can best be explained by reviewing some of the homeostatic control systems mentioned previously. In the regulation of carbon dioxide concentration, a high concentration of carbon dioxide in the extracellular fluid increases pulmonary ventilation. This, in turn, decreases the extracellular fluid carbon dioxide concentration because the lungs expire greater amounts of carbon dioxide from the body. In other words, the high concentration of carbon dioxide initiates events that decrease the concentration toward normal, which is negative to the initiating stimulus. Conversely, if the carbon dioxide concentration falls too low, this causes feedback to increase the concentration. This response also is negative to the initiating stimulus. |
|
In the arterial pressure-regulating mechanisms, a high pressure causes a series of reactions that promote a lowered pressure, or a low pressure causes a series of reactions that promote an elevated pressure. In both instances, these effects are negative with respect to the initiating stimulus. |
|
Therefore, in general, if some factor becomes excessive or deficient, a control system initiates negative feedback, which consists of a series of changes that return the factor toward a certain mean value, thus maintaining homeostasis. |
|
page 7 |
|
|
|
page 8 |
|
'Gain' of a Control System. The degree of
effectiveness with which a control system maintains constant conditions is
determined by the gain of the negative feedback. For instance, let us
assume that a large volume of blood is transfused into a person whose
baroreceptor pressure control system is not functioning, and the arterial
pressure rises from the normal level of 100 mm Hg up to 175 mm Hg. Then, let
us assume that the same volume of blood is injected into the same person when
the baroreceptor system is functioning, and this time the pressure increases
only 25 mm Hg. Thus, the feedback control system has caused a
'correction' of -50 mm Hg-that is, from 175 mm Hg to 125 mm Hg.
There remains an increase in pressure of +25 mm Hg, called the
'error,' which means that the control system is not 100 per cent
effective in preventing change. The gain of the system is then calculated by
the following formula: |
|
The gains of some other physiologic control systems are much greater than that of the baroreceptor system. For instance, the gain of the system controlling internal body temperature when a person is exposed to moderately cold weather is about -33. Therefore, one can see that the temperature control system is much more effective than the baroreceptor pressure control system. |
|
Positive Feedback Can Sometimes Cause Vicious Cycles and Death |
|
One might ask the question, Why do essentially all control systems of the body operate by negative feedback rather than positive feedback? If one considers the nature of positive feedback, one immediately sees that positive feedback does not lead to stability but to instability and often death. |
|
Figure 1-3 shows an example in which death can ensue from positive feedback. This figure depicts the pumping effectiveness of the heart, showing that the heart of a healthy human being pumps about 5 liters of blood per minute. If the person is suddenly bled 2 liters, the amount of blood in the body is decreased to such a low level that not enough blood is available for the heart to pump effectively. As a result, the arterial pressure falls, and the flow of blood to the heart muscle through the coronary vessels diminishes. This results in weakening of the heart, further diminished pumping, a further decrease in coronary blood flow, and still more weakness of the heart; the cycle repeats itself again and again until death occurs. Note that each cycle in the feedback results in further weakening of the heart. In other words, the initiating stimulus causes more of the same, which is positive feedback. |
|
|
|
|
|
Figure 1-3 Recovery of heart pumping caused by negative feedback after 1 liter of blood is removed from the circulation. Death is caused by positive feedback when 2 liters of blood are removed. |
|
Positive feedback is better known as a 'vicious cycle,' but a mild degree of positive feedback can be overcome by the negative feedback control mechanisms of the body, and the vicious cycle fails to develop. For instance, if the person in the aforementioned example were bled only 1 liter instead of 2 liters, the normal negative feedback mechanisms for controlling cardiac output and arterial pressure would overbalance the positive feedback and the person would recover, as shown by the dashed curve of Figure 1-3. |
|
Positive Feedback Can Sometimes Be Useful. In some instances, the body uses positive feedback to its advantage. Blood clotting is an example of a valuable use of positive feedback. When a blood vessel is ruptured and a clot begins to form, multiple enzymes called clotting factors are activated within the clot itself. Some of these enzymes act on other unactivated enzymes of the immediately adjacent blood, thus causing more blood clotting. This process continues until the hole in the vessel is plugged and bleeding no longer occurs. On occasion, this mechanism can get out of hand and cause the formation of unwanted clots. In fact, this is what initiates most acute heart attacks, which are caused by a clot beginning on the inside surface of an atherosclerotic plaque in a coronary artery and then growing until the artery is blocked. |
|
page 8 |
|
|
|
page 9 |
|
Childbirth is another instance in which positive feedback plays a valuable role. When uterine contractions become strong enough for the baby's head to begin pushing through the cervix, stretch of the cervix sends signals through the uterine muscle back to the body of the uterus, causing even more powerful contractions. Thus, the uterine contractions stretch the cervix, and the cervical stretch causes stronger contractions. When this process becomes powerful enough, the baby is born. If it is not powerful enough, the contractions usually die out, and a few days pass before they begin again. |
|
Another important use of positive feedback is for the generation of nerve signals. That is, when the membrane of a nerve fiber is stimulated, this causes slight leakage of sodium ions through sodium channels in the nerve membrane to the fiber's interior. The sodium ions entering the fiber then change the membrane potential, which in turn causes more opening of channels, more change of potential, still more opening of channels, and so forth. Thus, a slight leak becomes an explosion of sodium entering the interior of the nerve fiber, which creates the nerve action potential. This action potential in turn causes electrical current to flow along both the outside and the inside of the fiber and initiates additional action potentials. This process continues again and again until the nerve signal goes all the way to the end of the fiber. |
|
In each case in which positive feedback is useful, the positive feedback itself is part of an overall negative feedback process. For example, in the case of blood clotting, the positive feedback clotting process is a negative feedback process for maintenance of normal blood volume. Also, the positive feedback that causes nerve signals allows the nerves to participate in thousands of negative feedback nervous control systems. |
|
More Complex Types of Control Systems-Adaptive Control |
|
Later in this text, when we study the nervous system, we shall see that this system contains great numbers of interconnected control mechanisms. Some are simple feedback systems similar to those already discussed. Many are not. For instance, some movements of the body occur so rapidly that there is not enough time for nerve signals to travel from the peripheral parts of the body all the way to the brain and then back to the periphery again to control the movement. Therefore, the brain uses a principle called feed-forward control to cause required muscle contractions. That is, sensory nerve signals from the moving parts apprise the brain whether the movement is performed correctly. If not, the brain corrects the feed-forward signals that it sends to the muscles the next time the movement is required. Then, if still further correction is needed, this will be done again for subsequent movements. This is called adaptive control. Adaptive control, in a sense, is delayed negative feedback. |
|
Thus, one can see how complex the feedback control systems of the body can be. A person's life depends on all of them. Therefore, a major share of this text is devoted to discussing these life-giving mechanisms. |
|
Summary-Automaticity of the Body |
|
The purpose of this chapter has been to point out, first, the overall organization of the body and, second, the means by which the different parts of the body operate in harmony. To summarize, the body is actually a social order of about 100 trillion cells organized into different functional structures, some of which are called organs. Each functional structure contributes its share to the maintenance of homeostatic conditions in the extracellular fluid, which is called the internal environment. As long as normal conditions are maintained in this internal environment, the cells of the body continue to live and function properly. Each cell benefits from homeostasis, and in turn, each cell contributes its share toward the maintenance of homeostasis. This reciprocal interplay provides continuous automaticity of the body until one or more functional systems lose their ability to contribute their share of function. When this happens, all the cells of the body suffer. Extreme dysfunction leads to death; moderate dysfunction leads to sickness. |
|
References |
|
Adolph EF: Physiological adaptations: hypertrophies and superfunctions. Am Sci 60:608, 1972. |
|
Bernard C: Lectures on the Phenomena of Life
Common to Animals and Plants. |
|
Cabanac M: Regulation and the ponderostat. Int J Obes Relat Metab Disord 25(Suppl 5):S7, 2001. |
|
Cannon WB: The Wisdom of the Body. |
|
Conn PM, Goodman HM: Handbook of Physiology:
Cellular Endocrinology. |
|
Csete ME, Doyle JC: Reverse engineering of biological complexity. Science 295:1664, 2002. |
|
Danzler WH (ed): Handbook of Physiology, Sec 13:
Comparative Physiology. |
|
Dickinson MH, |
|
Garland T Jr, Carter PA: Evolutionary physiology. Annu Rev Physiol 56:579, 1994. |
|
Gelehrter TD, Collins FS: Principles of
Medical Genetics. |
|
Guyton AC: Arterial Pressure and Hypertension.
|
|
Guyton AC, Jones CE, Coleman TG: Cardiac
Output and Its Regulation. |
|
Guyton AC, Taylor AE, Granger HJ: Dynamics and
Control of the Body Fluids. |
|
Hoffman JF, Jamieson JD: Handbook of
Physiology: Cell Physiology. |
|
Krahe R, Gabbiani F: Burst firing in sensory systems. Nat Rev Neurosci 5:13, 2004. |
|
Lewin B: Genes VII. |
|
page 9 |
|
|
|
page 10 |
|
Masoro EJ (ed): Handbook of Physiology, Sec
11: Aging. |
|
Milhorn HT: The Application of Control Theory
to Physiological Systems. |
|
Orgel LE: The origin of life on the earth. Sci Am 271:76, 1994. |
|
Smith HW: From Fish to Philosopher. |
|
Thomson RC: Biomaterials Regulating Cell
Function and Tissue Development. |
|
Tjian R: Molecular machines that control genes. Sci Am 272:54, 1995. |
|
Politica de confidentialitate | Termeni si conditii de utilizare |

Vizualizari: 2033
Importanta: ![]()
Termeni si conditii de utilizare | Contact
© SCRIGROUP 2025 . All rights reserved